How many of you have floaters in your vision?
You know – those little (or sometimes bigger) black spots, dots, and squiggles that course through your vision that normally become more noticeable when you’re looking at a white/bright background?
Have you ever wondered what they are (other than annoying) and why you have them?
Let’s chat!
Floaters: In Focus
Ocular Anatomy
As normal, before we can fully dive into what floaters are, there needs to be a little bit of context – namely, knowledge of some ocular anatomy.
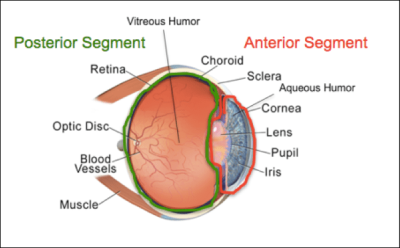
From those who have been following these posts, in my article “Why Does My Eye Doctor… Part 3” where I discuss the reason for the air puff test, I talk quite a bit about the anterior chamber (and segment) and the liquid, or aqueous, that fills it. For today, however, we’re going to be hopping further back in the eye, and going behind the lens to the posterior segment (highlighted in green in the picture below).
This back portion of the eye is made of several components (retina, optic nerve, choroid, other vasculature), but today’s focus is primarily on one: the vitreous.
Vitreous, or vitreous humor, is a jelly-like substance that functions to absorb shock, maintain the shape of the eye, keep the retina intact, and transfer molecules (like oxygen) from the front to the back of the eye.
In youth (generally), this jelly-like substance has a pretty uniform consistency – the fibers that make it up are evenly spaced, with water-loving molecules spread throughout to maintain proper water content and spacing.
However, with time, this spacing changes. The fibers that were once perfectly spaced begin to clump together, as the water component of the vitreous increases. These fiber clumps cast shadows on your retina as light comes in, causing you to see floaters!
Types of Floaters
While simple, normal, changes in the vitreous are the most common type/cause of floaters, there are others. For instance:
- In cases of ocular inflammation, there can be cells (specifically white blood cells) that end up in the vitreous. This is commonly referred to as vitritis, and may present with complaints of floaters.
- Sometimes when there is bleeding around the retina, the blood can escape into the vitreous, causing a vitreous hemorrhage. Patients at times report seeing red floaters in this situation.
- As the vitreous begins to clump together, it can put tension on the retina. Most of the time, this is focused around the optic nerve, where the vitreous is strongly attached. Eventually, the vitreous pulls enough and detaches, forming a c-shaped, or spiderweb-like floater that’s relatively close to the center of vision. This detaching of the vitreous from the retina is called a posterior vitreous detachment, and though it sounds really bad, it’s perfectly normal!
- In some cases, in conjunction with the vitreous pulling on the retina, a piece of the retina may actually tear off, forming either an operculated retinal hole, or a retinal tear (which then may lead to a retinal detachment).
Who gets floaters?
The short of it is – everyone! However, the number of floaters and the time of onset varies dramatically from person to person. As an example: I’d like to think I’m pretty young, but I have a lot of floaters – so many that I’ve been known to question if I’m seeing my floaters or my patients floaters during an exam, as well as wonder if I’m seeing bugs flying around or just some new floaters! My dad, on the other hand, says he rarely if ever notices floaters in his vision!
When to Be Concerned
While floaters are very common, sudden changes in floaters can indicate a problem (such as inflammation, bleeding, or detachment), in the back of the eye. For this reason, anyone who experiences a sudden increase in flashes and floaters should immediately contact their eye care provider!
If you learned something from this post, please share it with a friend or family member! If you liked it, please subscribe, or like my page on Facebook! And as always, if you have any questions or comments, please contact me – I’d love to hear from you!